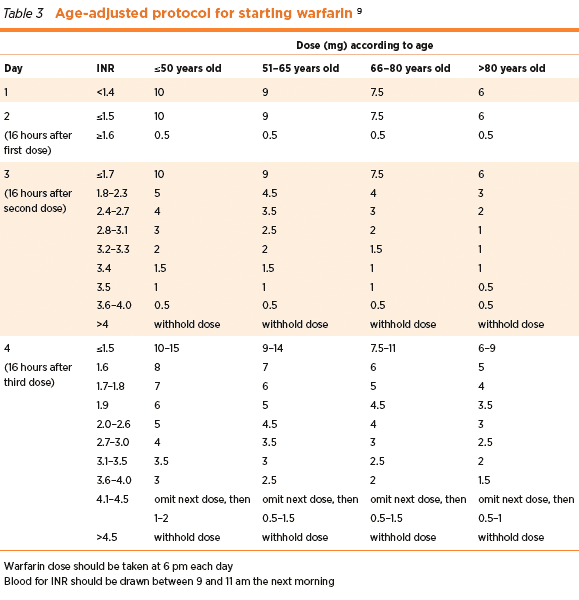
Patients were excluded if they were either taking any concurrent medication or had any chronic condition that may affect warfarin disposition or its pharmacologic activity, or excessive alcohol intake that could have affected anticoagulation response to warfarin. Inclusion criteria for patients used to validate the algorithm (designated as the validation cohort) were the ability to provide informed consent, age ≥ 18 years, and about to discontinue warfarin therapy. The inclusion and exclusion criteria of patients in the algorithm cohort have been previously reported. Where age in years n.CYP2C9: presence of CYP2C9 double variant (either *3*3, *3*2, or *2*2) = 1 and absence of double variant = 0, index INR (INR on day 1) w: weight in kg and n.com: number of comorbidities, including AF or other indication for warfarin therapy. This study aimed to validate the algorithm, using data from an independent cohort of patients who had discontinued warfarin therapy for a reason unrelated to surgery. Based upon the study results an algorithm was developed to predict the fall in INR in individual patients 5 days after warfarin cessation. These factors accounted for approximately 90% of the inter-individual variability in the rate of INR decline. In a recent study in adult patients who interrupted warfarin therapy prior to elective surgery, we demonstrated that the rate of INR decline following warfarin cessation was slower in patients with two CYP2C9 variant alleles, increasing age, weight and number of comorbidities and faster with greater INR value prior to warfarin withdrawal. 
Discontinuation of therapy too early may predispose the patient to thrombosis or stopping it too late may result in cancellation of the planned procedure due to risk of peri-operative bleeding. However, the anticoagulant activity of warfarin subsides at different rates among different patients, thus withholding warfarin for 5 days may not result in restoration of normal coagulation in all patients. Patients on warfarin are required to stop treatment for a fixed period (5 days according to local guidelines) prior to an invasive procedure, in order to minimise the risk of peri-operative bleeding. The use of this easily adoptable algorithm can reduce cancellation or delays of planned surgical procedures. The algorithm can accurately predict the INR decline following warfarin cessation in individual adult patients. The algorithm was precise, with low degree of bias and variance of the prediction error. There was a strong correlation between the decline in INR by day 5 and that predicted from the algorithm for the 117 patients (r = 0.949, p < 0.001). The predicted INR decline (INR day 1–INR day 5) was compared to the observed one (where an INR check on day 5 was unavailable, INR was estimated using a linear approximation model). 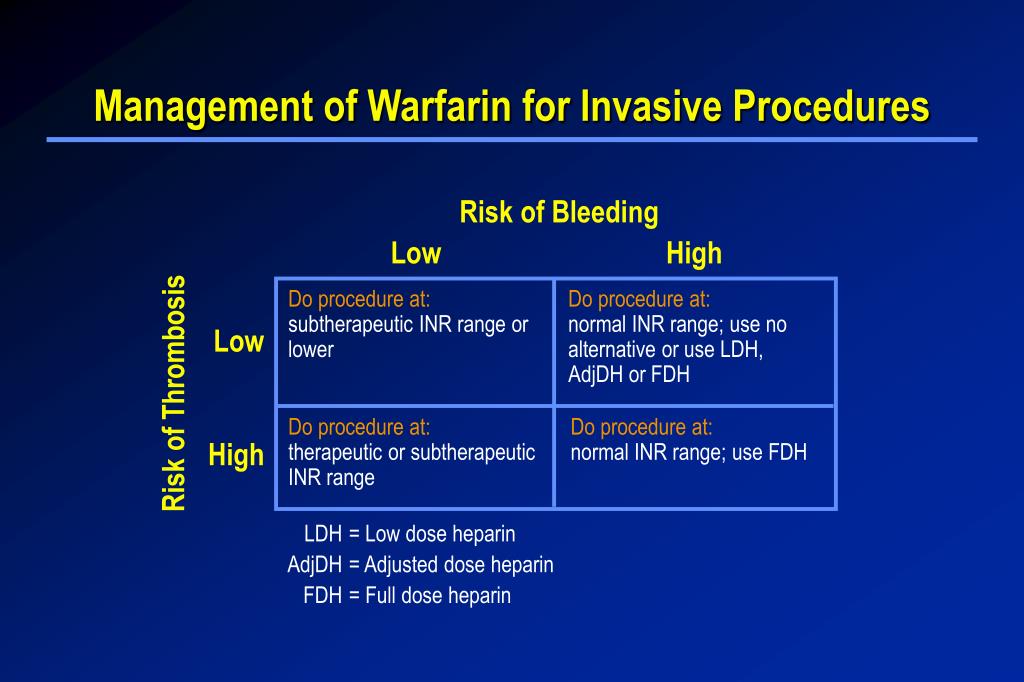
INR values for subsequent 9 days and CYP2C9 genotype were available. An independent cohort of patients completing a short course of warfarin took part in the study. The current study validated the algorithm. Subsequently, we developed an algorithm which predicts INR decline in individual patients after 5 days of warfarin cessation. In a recent study in patients awaiting surgery, following warfarin cessation the INR declined slower over time in those with two CYP2C9 variant alleles, increasing age, weight and number of comorbidities and that INR decline was faster in those with higher maintenance INR value. However, the anticoagulant effect of warfarin subsides at different rates among different patients, exposing some to increased risk of either thrombosis or bleeding. Patients on warfarin are required to withdraw from treatment for a fixed period (normally 5 days) prior to an invasive procedure.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
